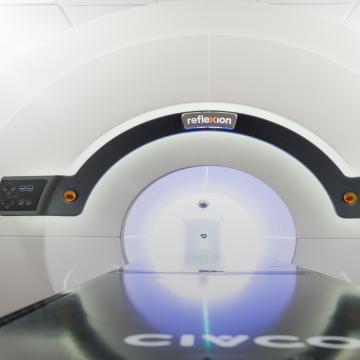
Lutathera PRRT
Lutathera PRRT, a targeted therapy for neuroendocrine tumors of the small intestine and pancreas, received approval from the Food and Drug Administration in late January 2018.
The approval of Lutathera came on the heels of aHHa clinical study called NETTER-1. The trial evaluated the medicine for treating patients with somatostatin-receptor-positive neuroendocrine tumors of the small intestine with advanced, metastatic disease.
Lutathera PRRT is a targeted radiation treatment, designed to attack cancer cells while minimizing harm to healthy tissue. The “PRRT” stands for “peptide receptor radionuclide therapy.”
City of Hope is one of the first centers nationwide to offer Lutathera as part of our patient-centered team approach to fighting gastroenteropancreatic neuroendocrine tumors.
People confronted with these rare malignancies have had a limited number of options to control them. With this powerful addition to the anticancer arsenal, City of Hope’s multidisciplinary compassionate care team swiftly provided Lutathera PRRT as a new option for combating gastrointestinal neuroendocrine tumors.
Because we believe that cancer patients — no matter how uncommon a disease they face — shouldn’t have to wait on better treatments.
City of Hope is one of the few facilities designated a comprehensive cancer center by the National Cancer Institute.

Our developments in the areas of breakthrough cancer drugs, bone marrow transplants and CAR T cell therapy are recognized internationally.

Our leadership in research and innovation continually enhances our ability to provide novel and differentiated approaches to cancer care.

Alexander Jung, M.D., is a diagnostic radiologist focusing on specialized imaging procedures, including high contrast ultrasound imaging and full body imaging.
Daneng Li, M.D., is a medical oncologist specializing in geriatric oncology and treating gastrointestinal cancers.

Maria Parayno, M.D., is an assistant clinical professor in the Division of Nuclear Medicine, Department of Diagnostic Radiology.

Dave M. Yamauchi, M.D., is the chief of the Division of Nuclear Medicine and a diagnostic radiologist specializing in interventional radiology.