Radiation Therapy for Head and Neck Cancers
The standard treatment of head and neck cancers often includes combined modality therapy involving surgery followed by postoperative radiation or organ preservation with definitive chemotherapy and radiation, without the need for surgery.
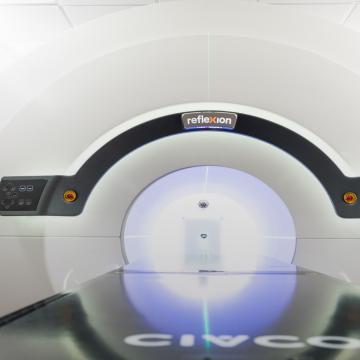
Advances in image-guided radiation therapy have allowed us to deliver more intense doses of radiation in a more focused area of the body, increasing the treatment’s effectiveness against cancer and minimizing its impact on surrounding structures, including critical structures such as salivary glands, spinal cord, brainstem and swallowing muscles.
At City of Hope, we have been treating head and neck cancers using helical TomoTherapy since 2004. Our team has extensive experience in planning and delivering such treatment.
When you come to City of Hope, you automatically gain access to an unparalleled array of support services to help you and your loved ones take each step during and after head and neck cancer treatment.
City of Hope is one of the few facilities designated a comprehensive cancer center by the National Cancer Institute.

Our developments in the areas of breakthrough cancer drugs, bone marrow transplants and CAR T cell therapy are recognized internationally.

Our leadership in research and innovation continually enhances our ability to provide novel and differentiated approaches to cancer care.