Breast Cancer Treatment and Survival Rate
April 10, 2025
This page was reviewed under our medical and editorial policy by Nikhila Kethireddy, M.D., assistant clinical professor, and Susan Yost, Ph.D., staff scientist, Department of Medical Oncology & Therapeutics Research, City of Hope® Cancer Center Duarte
Following a breast cancer diagnosis, the care team will work with patients to create a personalized treatment plan based on their cancer type and stage, as well as their overall health and treatment goals.
Who Treats Breast Cancer?
Treating breast cancer involves a multidisciplinary care team of experts who work together to provide personalized, targeted breast cancer treatment options. The patient’s care team may include the following medical professionals.
- Surgical oncologists who treat cancer using surgery
- Radiation oncologists who treat cancer using radiation (electromagnetic waves or particles)
- Medical oncologists who treat cancer using hormone therapy, targeted drug therapy, chemotherapy (drugs that destroy cancer cells), immunotherapy (substances that elevate or suppress the immune system) and other breast cancer medications
- Endocrinologists specializing in diseases of the endocrine system, which includes glands and organs that make and release hormones
- Plastic or reconstructive surgeons trained to remove and repair tissue and reconstruct the breasts
- Interventional radiologists who specialize in minimally invasive radiology procedures using imaging tests
- Pathologists trained to study tissue from biopsies in the laboratory in order to diagnose, stage and grade cancer
- Anesthesiologists trained to provide drugs during surgery or medical procedures to numb nerves or put patients to sleep to alleviate pain
- Pharmacists, who are licensed medical professionals trained in managing prescribed medications and substances to ensure patient safety
- Supportive medicine providers who help patients manage cancer symptoms and cancer treatment side effects
Factors That Affect Treatment Options
The patient’s multidisciplinary care team works together to decide on appropriate treatments for breast cancer.
Treatment recommendations are based on a number of factors, including:
- Cancer stage, which gauges how much cancer is in the patient’s body and how far it has spread (metastasized)
- The patient’s treatment goals and preferences
- Whether the patient has gone through menopause
- Whether the cancer is affecting major organs, such as the lungs or liver
- How fast the cancer is growing, which includes measuring its grade (how abnormal the cells look under a microscope)
- If the cancer has recurred (returned)
- The presence of certain genetic mutations (changes) in the cancer cells
- The presence of estrogen and progesterone hormone receptors on the cancer cells, known as estrogen-receptor (ER) positive or progesterone-receptor (PR) positive breast cancer
- The presence of higher levels of the protein HER2 on the cancer cells, which helps them grow and spread quickly
Breast Cancer Treatments
Some of the most common treatments for breast cancer are surgery, medications, radiation therapy and hormone therapy. Which course of care is appropriate for each patient depends on several factors, including the type of breast cancer they have, the cancer stage and their desired outcomes.
Breast Cancer Surgery
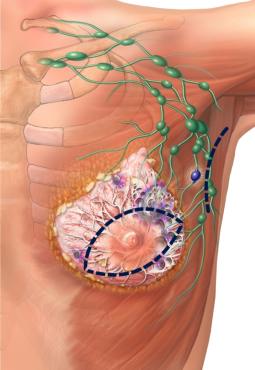
Breast cancer surgery is a common treatment option for most breast cancer patients. Depending on the tumor’s size, location and spread, doctors may recommend a lumpectomy or a mastectomy.
Lumpectomy
Lumpectomy is the surgical removal of a tumor, the surrounding breast tissue and, sometimes, nearby lymph nodes. This option is often used for small, early-stage tumors and seeks to conserve as much of the breast as possible. A lumpectomy is usually followed by radiation therapy, and sometimes by hormone therapy or chemotherapy with or without other targeted therapies.
Mastectomy
Mastectomy is the surgical removal of one or both breasts, along with nearby lymph nodes. Mastectomies are sometimes performed as a risk-reduction procedure for women with a high risk for developing breast cancer.
The surgical team may offer advanced surgical options like a nipple-sparing mastectomy or skin-sparing mastectomy.
Lymph Node Removal
Lymph node removal surgery includes the removal of one or more lymph nodes. They may be removed from under the arm or from the area surrounding the breastbone or collarbone. The number of lymph nodes removed depends on how far the cancer has spread.
A surgeon may perform a sentinel lymph node biopsy to remove a smaller number of lymph nodes or an axillary lymph node dissection if more lymph nodes need to be removed.
If cancer is present in lymph nodes under the arm, the disease may have already spread to other parts of the body. A pathologist will look at these lymph nodes under a microscope to help the doctor understand the extent of the cancer’s spread.
Breast Reconstruction and Microsurgery
Breast reconstruction surgery rebuilds the shape of the breast after a mastectomy. Some of these procedures are performed at the same time as the mastectomy (known as immediate reconstruction), while others are performed later (known as delayed reconstruction). Although the breast shape is restored, sensation in the breast and the nipple usually remains limited. In most cases, surgeons use a flap of tissue from elsewhere to rebuild the shape of the breast.
When cancer surgery is combined with plastic surgery, it is called oncoplastic surgery. This typically involves reshaping the breast at the same time as the initial surgery. In some cases, surgery is performed on a healthy breast so that the shape of both breasts matches.
As an alternative to reconstruction, some women prefer to wear prosthetic breast forms inside their bra or attached to their body, while others choose to have a flat chest.
Radiation Therapy for Breast Cancer
Radiation therapy for breast cancer uses high-energy rays (such as X-rays) or particles to destroy cancer cells. The care team may recommend radiation alone, or in combination with other treatments like surgery, depending on factors such as the type of cancer, whether it has spread and the patient’s age. Radiation therapies are often used:
- After breast-conserving surgery, to help lower the chance that the cancer will come back in the breast or nearby lymph nodes
- After a mastectomy, especially if the cancer was larger than two inches, or if cancer is found in the lymph nodes
- If cancer has spread to other parts of the body, such as the bones or brain, and is causing symptoms
Drug Therapy for Breast Cancer
A number of drug therapy treatments may help the body fight breast cancer by killing the cancer cells or stopping their growth and spread.
Chemotherapy for Breast Cancer
Chemotherapy targets all rapidly dividing cells, including breast cancer cells. Breast cancer chemotherapy treatment consists of cancer-killing drugs that can be injected or taken by mouth. These drugs travel through the bloodstream to reach cancer cells wherever they are in the body. Chemotherapy is often recommended:
- After surgery (called adjuvant chemotherapy), to try to kill cancer cells that may have been left behind or spread
- Before surgery (called neoadjuvant chemotherapy), often when a cancer is too big to be removed at the time of diagnosis
- For advanced breast cancer
Targeted Therapy for Breast Cancer
Targeted therapy for breast cancer selectively attacks cancer based on specific characteristics of the breast cancer cells. Biomarker tests help identify these characteristics, which include certain proteins, receptors, or gene arrangements or changes (mutations).
If a biomarker test shows the presence of one of these markers, breast cancer drugs may be used to target it in order to help slow cancer cell division, growth or spread. Examples of biomarker tests include the HER2 protein test and the estrogen and progesterone hormone receptor test.
Immunotherapy for Breast Cancer
Immunotherapy for breast cancer stimulates a patient’s immune system to attack the cancer cells from within.
Which drug therapies are best for a patient depends on a variety of factors, including the type and stage of breast cancer, previous treatments and their overall health and goals. Genetic testing may also help identify treatments that are more appropriate for each patient.
Hormone Therapy for Breast Cancer
About 3 out of 4 breast cancers rely on hormones like estrogen and/or progesterone to fuel their growth. Drugs that decrease endocrine (or hormone) production can help slow or halt the disease. Breast cancer hormone therapy is most often used after surgery to reduce likelihood of cancer recurrence, but may be used in other settings as well.
Breast Cancer Survival Rate
Breast cancer survival rates depend on many factors, including the stage at which the disease is diagnosed, the type of breast cancer, the presence of certain biomarkers such as HER2, and the patient’s age and overall health.
One way to measure the survival rate of breast cancer is to compare how many women with the same stage and type of cancer are alive after five years to women in the general population. This is known as the five-year relative survival rate.
For breast cancer, the National Cancer Institute lists the overall five-year relative survival rate between 2015 and 2021 as 91.7%. It varies significantly by stage.
Localized cancer (cancer remains in the breast): 100%
Regional cancer (cancer has spread to nearby lymph nodes or structures): 87.2%
Distant cancer (cancer has spread to structures throughout the body): 32.6%
Some types of breast cancer are more aggressive and more challenging to remove.
Women diagnosed with inflammatory breast cancers had a lower overall five-year relative survival rate of 40% between similar years (2015 and 2021), according to the American Cancer Society (ACS).
Women diagnosed with triple-negative breast cancer had an overall five-year relative survival rate of 78% between similar years (2015 and 2021), according to ACS.
New treatment options are being researched and developed aimed at positively impacting breast cancer survival outcomes.
The City of Hope Difference
The world-class surgical team at City of Hope has expertise in some of the most innovative approaches to breast reconstruction, including those listed below.
Rib-sparing reconstruction: This procedure allows surgeons to access mammary (breast) blood vessels and reconnect them to the tissue being used to reconstruct the breast, helping improve surgical outcomes.
DIEP (deep inferior epigastric perforator) flap: This approach to abdominal flap-based reconstruction preserves muscle tissue and function of nearby nerves (relative innervation).
Abdominal perforator exchange (APEX) flap surgery: This procedure is an abdominal flap-based reconstruction that does not remove muscle tissue, thus helping preserve nerve functioning and reduce complications at the donor site.
Posterior thigh-based profunda artery perforator (PAP) flap surgery: This approach offers an alternative to using an abdominal flap for patients who are slim or have had prior major abdominal surgery or liposuction that limits available abdominal tissue.
Breast reinnervation with breast reconstruction surgery: This procedure follows either conventional or nipple-sparing mastectomies, during which the surgeon dissects and reconnects one of the body’s intercostal sensory nerves — an approach that has been highly successful in restoring sensation both to the breast mound and nipple-areolar complex.
In addition, the City of Hope® breast cancer surgical team has extensive experience in a variety of lymphatic reconstruction and bypass techniques. This is important because lymphedema — the retention of lymph fluid and swelling after surgery or radiation — affects approximately 1 in 5 breast cancer survivors, with incidence rates as high as 30% to 60% reported in survivors with axillary lymph node dissection.
Once lymphedema has become chronic, it is typically not curable. The good news is that early diagnosis and treatment, along with proper surgical techniques, may help improve fluid flow and prevent long-term side effects and tissue damage.
City of Hope’s advanced lymphatic function preservation microsurgery techniques include:
Robotic vascularized lymph node transplant, in which autologous lymph nodes are transplanted from the abdomen to replace lymph nodes removed during treatment.
Lymphaticovenous anastomosis (LVA), a bypass procedure during which lymph fluid is redirected to small veins with virtually no blood loss (typically an outpatient procedure that takes four to six hours, with patients remaining fewer than 24 hours for observation).
American Cancer Society. Treating breast cancer, 2024.
https://www.cancer.org/cancer/types/breast-cancer/treatment.htmlAmerican Cancer Society. Health professionals who are part of a cancer care team, August 8, 2024.
https://www.cancer.org/cancer/managing-cancer/finding-care/health-professionals-associated-with-cancer-care.htmlNational Cancer Institute, NCI Dictionary of Cancer Terms. Radiology.
https://www.cancer.gov/publications/dictionaries/cancer-terms/def/radiologyNational Cancer Institute, NCI Dictionary of Cancer Terms. Radiation.
https://www.cancer.gov/publications/dictionaries/cancer-terms/def/radiationNational Cancer Institute, NCI Dictionary of Cancer Terms. Chemotherapy.
https://www.cancer.gov/publications/dictionaries/cancer-terms/def/chemotherapyNational Cancer Institute, NCI Dictionary of Cancer Terms. Immunotherapy.
https://www.cancer.gov/publications/dictionaries/cancer-terms/def/immunotherapyNational Cancer Institute, NCI Dictionary of Cancer Terms. Endocrine system.
https://www.cancer.gov/publications/dictionaries/cancer-terms/def/endocrine-systemAmerican Cancer Society. Treatment of breast cancer by stage, September 18, 2019.
https://www.cancer.org/cancer/types/breast-cancer/treatment/treatment-of-breast-cancer-by-stage.htmlAmerican Cancer Society. Breast cancer stages, November 8, 2021.
https://www.cancer.org/cancer/types/breast-cancer/understanding-a-breast-cancer-diagnosis/stages-of-breast-cancer.htmlNational Cancer Institute, NCI Dictionary of Cancer Terms. Grade.
https://www.cancer.gov/publications/dictionaries/cancer-terms/def/gradeAmerican Cancer Society. Breast cancer hormone receptor status, November 8, 2021.
https://www.cancer.org/cancer/types/breast-cancer/understanding-a-breast-cancer-diagnosis/breast-cancer-hormone-receptor-status.htmlAmerican Cancer Society. Breast cancer HER2 status, August 25, 2022.
https://www.cancer.org/cancer/types/breast-cancer/understanding-a-breast-cancer-diagnosis/breast-cancer-her2-status.htmlAmerican Cancer Society. Lymph node surgery for breast cancer, January 3, 2023.
https://www.cancer.org/cancer/types/breast-cancer/treatment/surgery-for-breast-cancer/lymph-node-surgery-for-breast-cancer.htmlNational Cancer Institute. Biomarker testing for cancer treatment, December 14, 2021.
https://www.cancer.gov/about-cancer/treatment/types/biomarker-testing-cancer-treatmentNational Cancer Institute. Tumor marker tests in common use, December 7, 2023.
https://www.cancer.gov/about-cancer/diagnosis-staging/diagnosis/tumor-markers-listAmerican Cancer Society. Targeted drug therapy for breast cancer, January 22, 2024.
https://www.cancer.org/cancer/types/breast-cancer/treatment/targeted-therapy-for-breast-cancer.htmlAmerican Cancer Society. Survival rates for breast cancer, January 17, 2024.
https://www.cancer.org/cancer/types/breast-cancer/understanding-a-breast-cancer-diagnosis/breast-cancer-survival-rates.htmlAmerican Cancer Society. Inflammatory breast cancer, March 1, 2023.
https://www.cancer.org/cancer/types/breast-cancer/about/types-of-breast-cancer/inflammatory-breast-cancer.htmlAmerican Cancer Society. Triple-negative breast cancer, March 1, 2023.
https://www.cancer.org/cancer/types/breast-cancer/about/types-of-breast-cancer/triple-negative.html